Quenton Rashawn Bubb continues to value the complex, complementary nature of work on parallel paths -- not just as a musician/academic, but now on the path to his career.
Category: Patient Care
Research explores liability risk of using AI tools in patient care
As the health care industry grapples with the best way to use artificial intelligence technologies to improve care, many clinicians may wonder what happens if patients are harmed, and who should be held liable.
Sick of being sick? As respiratory viruses roar back, experts offer guidance
Nationwide, the percentage of health care visits for flulike symptoms ticked up above the baseline at the start of November and has remained elevated ever since, according to the Centers for Disease Control and Prevention.
More kids are being hospitalized for eating disorders — researchers learned why
Over the last decade, physicians have taken a broader view of adolescent eating disorders, thanks to a growing recognition of the variety of disordered eating patterns that can harm patients’ health, especially their heart function.
2023 recap: Stories and videos that most connected with our readers
We share the stories and videos published in 2023 on our News Center, Scope and Stanford Medicine magazine sites that resonated most with our readers online and on social media.
The endometriosis enigma: What to know about this disruptive disease
Despite the fact the disease greatly reduces the quality of many women’s lives, endometriosis remains understudied.
Can art aid in healing? Portrait Project is using AI, traditional art to find out
Stanford Medicine researchers are helping patients use AI image-generation software as part of a unique study that aims to quantify how creating art aids patients in their recovery.
As seasons change, so does the guidance around antibiotics: Here’s what you need to know now
Clinical fellow Alex Zimmet, MD, a member of Stanford Medicine’s antimicrobial stewardship team, discusses why antibiotic overuse is a problem and how you can help combat it.
Do you sound like you? Gender-affirming voice therapy allows people to speak authentically
Why is it important to offer gender-affirming voice therapy or surgery? We spoke with experts on all sides of the equation.
A veteran serving veterans: Orthopaedic surgeon reflects on time in military, medicine
A proud veteran and surgeon, Constance Chu leads the Joint Preservation Center and Sports Medicine program at the Palo Alto VA.
How one blind genetic counselor is doing her part to address ableism
Many people mistakenly assume that because Ronit Mazzoni has been blind since birth, her career choice must have been related to her condition.
The time ‘is now, in the beginning’: How do we ensure AI tools aren’t biased?
New artificial intelligence tools have the potential to revolutionize health care. But Stanford researchers argue that disparities could worsen without intervention now.
AI, medicine and race: Why ending ‘structural racism’ in health care now is crucial
Health care providers must reckon with inherent race-based biases in medicine, which can reinforce false stereotypes in algorithms and lead to improper treatment recommendations or late diagnoses.
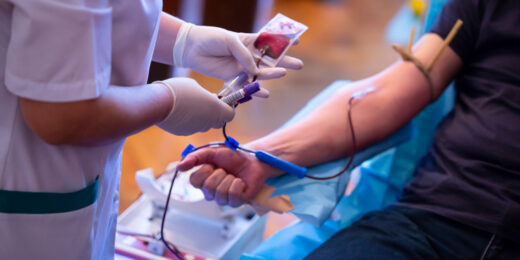
New policy is taking sexual orientation, gender out of blood donor equation
New guidelines will continue to ensure the safety of the nation's blood supply, according to the Food and Drug Administration.
Unconventional Paths: How archaeology inspired a path to family medicine
Bright Zhou learned from an interest in studying ancient DNA how storytelling is at the root of good family medicine.
Native American med student uses education to serve her community
Medical student Melissa Eidman speaks to her motivation to pursue medicine and how it intertwines with her Native heritage.