A patient I'll call Jason Greene is not taking his diabetes lying down.
Greene has cleared the hurdle of the packed waiting room. He has seen a physician and had several tests performed. However, unlike many other patients, he still wears his street clothes and is sitting upright in a comfortable treatment chair that resembles a living room armchair. He is a new breed of emergency department patient: a vertical one.
First implemented as a test model in September 2014, the Stanford Emergency Department "vertical flow model," which replaces horizontal stretchers with comfortable chairs, has proven successful in maximizing existing space and reducing length of stay, according to a recent study in the Journal of Emergency Nursing. And thanks to an especially virulent flu season, the extra space couldn’t be more welcome.
Like many emergency department's nationwide, Stanford has seen a 4 to 8 percent growth each of the past several years. A facility built in 1976 to accommodate 40,000 patients a year, instead hosted more than 73,500 visits in 2017, according to Patrice Callagy, director of emergency services at Stanford Health Care. While the department has gained some additional square footage, the patient volumes have grown more. A typical day brings an average of 200 patients; and during the flu season, that average recently swelled to 250-260 per day, department records show.
The numbers beg the question – how do you treat a growing number of patients in the same space, while protecting the patient experience and elevating care?
To understand the answer, it helps to know that emergency department patients are assigned a ranking from one to five based on the severity of their condition. An Emergency Severity Index (ESI) of 1 is life-threatening. An ESI of 5 is the least urgent.
ESI 3 is the most common category; ESI 3 patients require more than one resource or test, but their conditions can vary significantly. Traditionally, ESI 3 patients are placed in hospital beds in hospital gowns for assessment, treatment, and to await tests. However, not all patients need to lie down.
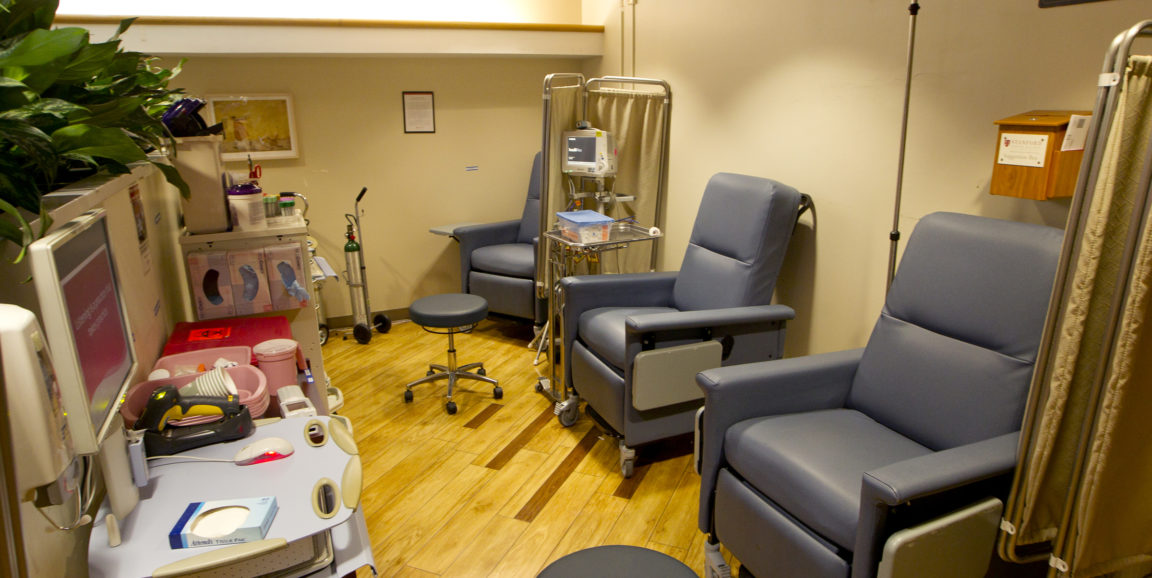
The solution was to “go vertical,” replacing some hospital beds with chairs to create a space that would accommodate up to 20 patients, compared with 10 previously.
A furniture swap is a seemingly simple solution until you take into account the need for patient privacy and access to testing equipment. The emergency department had to create and train staff on new work flows. Vertical patients are first brought to a private room to describe their medical history, receive a physical examination, and undergo some laboratory work. They return to the vertical zone for diagnostic testing and re-evaluation as needed. IV infusions and medications can be administered in the location as well.
As a result, the average length of stay for patients in the vertical zone shrank from 384 minutes to 270 minutes. Multiplied by the 2,701 patients in the zone during the six months of the study resulted in a savings of more than 5,000 patient hours, or 213 days.
The new Stanford Hospital, set to open in late 2019, will offer a larger emergency department. The new facility will feature several innovations tested in the current building – including the vertical flow model.
Photo by Norbert von der Groeben