Last week, I learned that among the earliest documented forms of birth control was lint.
That's right. Lint. And gum, and honey. These were some of humanity's first (think 1500 BC) attempts at quashing untimely or unwanted pregnancy.
At the 8th Women's Health Forum, which is put on each year by the Stanford WSDM Center, Kate Shaw, MD, a clinical associate professor of obstetrics and gynecology at Stanford, spoke and brought the history and evolution of contraception to center stage. "In year 600, we continue to see documentation of other ways to prevent pregnancy -- coitus interruptus, the withdrawal method," Shaw said during her talk. "Those traveling on long journeys would try to prevent pregnancy in their camels by putting stones in the camels' uterus. This was also applied to women."
My, how far we've come.
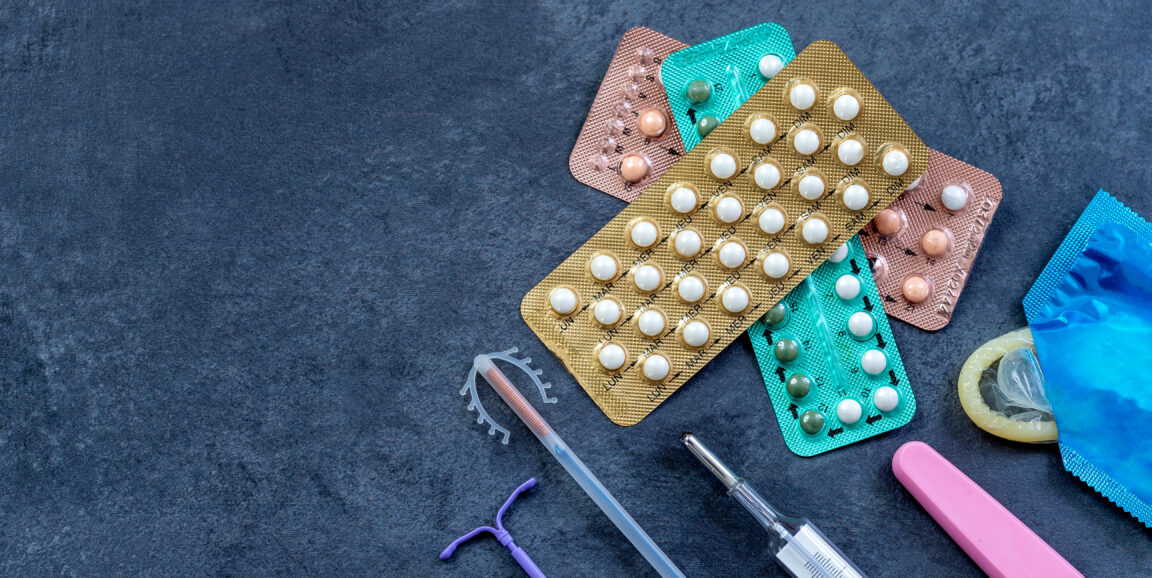
That stone, for all intents and purposes, was a first go at a modern form of long-term contraception called an intrauterine device, or IUD. Today, thankfully, women are offered a plethora of birth control options: the pill, IUDs, condoms, implants that sit just under the skin of the upper arm, the patch. And these are just some of the options, each of which have a variety of sub-choices within them.
But the freedom to exercise family planning, with so many options, was hard-won.
In the 1800s, two opposing movements bubbled up: On one side, women began openly expressing their want for birth control. But others argued that contraception was immoral and promoted prostitution. In 1870, the Comstock Act, a set of federal acts outlawing the use of the U.S. postal service to mail anything sex-related, including contraception, passed. Though numerous attempts to repeal the laws were made, it wasn't until more than a century later that the ban on mailing contraceptives was removed from law.
In the 1960s, activist Margaret Sanger (who essentially founded what is now today's Planned Parenthood) and philanthropist Katharine McCormick recruited a scientist by the name of Gregory Pincus, PhD, to co-invent the first version of "the pill."
And so began modern-day contraception. But there were still hangs up. The period from 1960 to 1980, Shaw explained, was filled with morphing laws regarding birth control use and education, for both married and unmarried women. Eventually it was accepted that married women had "the right to privacy" in regard to contraception and contraception education. But in the early 70s, a professor named William Baird talked to a classroom of unmarried women about contraception and at the end, provided a woman with a "contraceptive foam" that acts as a spermicide. He was charged with a crime. The case was taken to the Supreme Court, and the landmark decision to uphold and extend the right to privacy to unmarried women was made.
"So finally, everyone had the right to privacy and the right to access information about birth control," Shaw told the audience. "Today, with the Affordable Care Act, which established that all contraception methods should be available at no cost to women, women should have unrestricted access to contraception." That's an enormously different practice compared to the norms even less than 50 years ago, Shaw commented.
Shaw said there are so many birth control options for women today that it can be overwhelming. At a doctor's appointment where a woman might have 15 minutes to decide what kind of contraception she wants, they often opt for what's familiar -- perhaps going for what they've heard works for friends or family.
It's why, Shaw said, that she and many of her colleagues are now organizing contraceptive options on a new chart, based on efficacy. Those at the top -- IUDs and in-arm implants -- are the most effective, those toward the middle or bottom -- the pill or condoms -- less so. (Though don't be fooled. The ones toward the middle or bottom are often potent options for pregnancy prevention, but they're options that require an every-day oral ingestion, or application during sex -- both of which introduce opportunity for error).
Shaw also said that along with a new way to present the information, it's important to emphasize that no birth control is one-size fits all. She pointed out that women may benefit from trying more than one in an effort to find what works best for them.
Photo by JPC-PROD