A robotic surgical assistant known as ROSA™ recently helped experts at Lucile Packard Children's Hospital Stanford prepare for a minimally-invasive surgery to alleviate a little girl's seizures.
The surgery removed small areas of Brynn Mulrooney's brain where her seizures originated, all without harming nearby brain centers she needs to speak and smile. Before this treatment, even with epilepsy medications, Brynn was having up to 12 seizures per day.
When a prolonged seizure landed Brynn, now 7, in the hospital, her doctors began planning a way to use lasers to vaporize brain areas where the seizures began.
To do this safely, the team first needed to create precise maps of Brynn's brain. They used the Synaptive Medical platform to combine results from several brain-imaging tests, producing a detailed 3D map of Brynn's brain structure.
After that, with ROSA™ the robot, pediatric neurosurgeon Gerald Grant, MD, drilled tiny holes at carefully chosen locations in Brynn's skull. He then placed electrodes for a procedure called stereo EEG that would provide a detailed road map of the electrical activity in her brain. The hospital's story about Brynn explains what happened next:
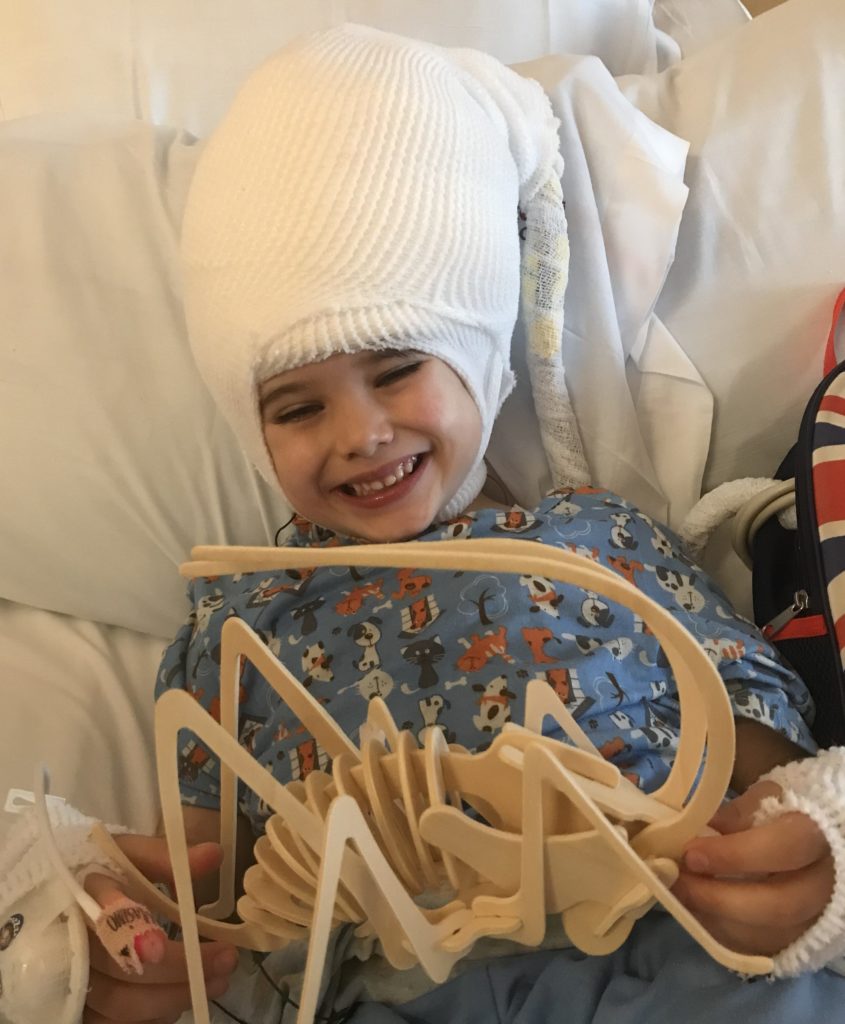
The electrodes stayed in place for two weeks, under a large head wrap, while doctors stimulated various electrodes waiting for seizures.
... The final step was the minimally invasive brain surgery to cure the seizures. First, doctors integrated the 3D imaging and electrical road map in the intraoperative MRI. Next, Dr. Grant precisely guided the laser to the target. When the laser was turned on, he was able to see the heat map generated by the laser, using MRI to ablate tiny targets deep in the brain.
"We brought together multiple innovative technologies to achieve the best possible outcome for Brynn," Dr. Grant says. "Brynn's deep targets were surrounded by areas of high real estate which were super important for her speech. It's a huge advance for us to travel right up against deep highways in the brain to ablate an area causing the seizures that was the size of a walnut."
Photos courtesy of the Mulrooney family




