Remote primary care has taken off during the COVID-19 pandemic -- a shift in practice that helps patients and physicians avoid spreading the coronavirus. But a Stanford Medicine researcher has found a downside: Many patients aren't getting routine tests that help determine their risk of heart disease and stroke.
Randall Stafford, MD, a professor of medicine, and his colleagues compared primary care visits conducted in the United States during the second quarter of 2020 with those that took place in the second quarters of 2018 and 2019.
In their article, published recently in JAMA Network Open, they noted that in 2020, the number of in-person primary care visits dropped by about half. Remote visits increased, but not enough to make up the difference: There were 21% fewer visits overall for the second quarter in 2020.
The researchers also found that the number of patients receiving blood pressure measurements dropped by 50%, and the number getting cholesterol tests decreased by 37%.
"The good news was we didn't have a complete cessation of physician visits," Stafford told me. "But there were fewer visits overall and less comprehensive evaluation."
Critical tests for prevention
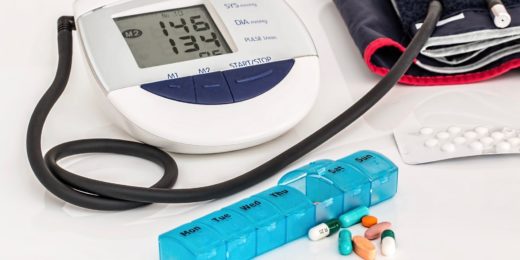
High blood pressure and elevated cholesterol are risk factors for heart disease and stroke, so testing for them is critical for prevention. Both conditions can improve with medications and lifestyle changes.
In their study, the researchers looked at blood pressure readings and cholesterol checks because they are common measurements taken during or in conjunction with primary care visits.
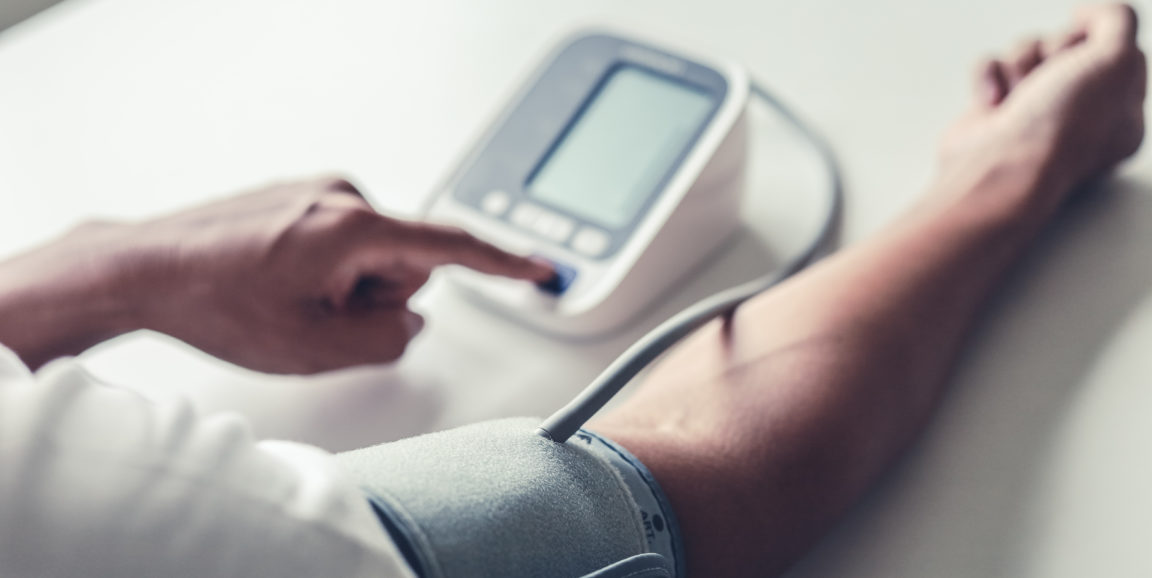
The researchers attributed the lower rate of the measurements to the increase in virtual visits. Unless patients have monitors at home, blood pressure can't be measured via telemedicine. And a cholesterol check must take place in person, as it usually requires a blood draw.
Stafford said blood pressure and cholesterol levels may be on the rise during the pandemic. "It's almost ubiquitous, what I'm hearing from patients," he said. "They say, 'I've gained some weight' or 'I'm not as active as I was before.'"
"It's possible that more people are developing greater risk for heart disease and stroke at this time when fewer people are being checked," he said.
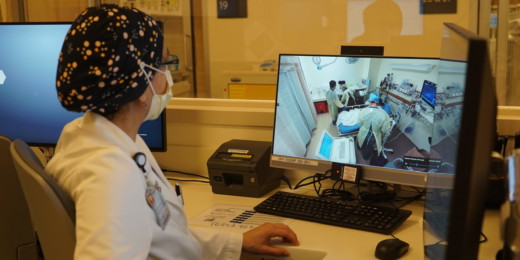
Practicing more effective telemedicine
Stafford said he hopes the research encourages primary care physicians to use telemedicine more effectively. This could mean reserving remote visits for certain patients, such as those who are adept at managing chronic conditions and can take measurements at home. Advances in home monitoring systems, such as watches that measure heart rate, will open virtual visits to more patients, he predicted.
Physicians can also learn how to better examine patients remotely, Stafford noted. For example, he uses a technique for virtual visits with urinary tract infection patients: He tells them to punch themselves in the lower back (if it hurts, that could be a kidney infection).
However, Stafford said, there are always patients who need to come in for an examination -- those with lung issues, for example, require an evaluation with a stethoscope.
He added that many patients, especially those with mobility or transportation problems, are grateful to have a video visit. For that reason, he believes virtual visits will remain a part of medical practice even when the pandemic no longer discourages in-person visits.
"Telemedicine is here to stay," Stafford said, "so we need to figure out the best ways to use it."
Photo by Watercolor_Concept