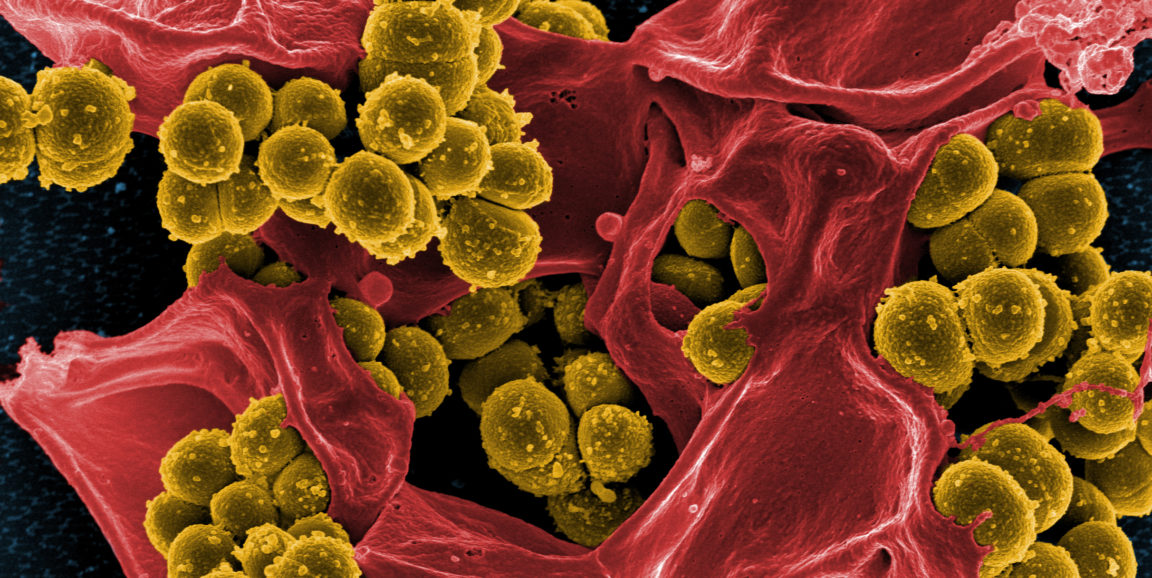
There are plenty of creatures that are fine to have around as long as they don't get inside your house: cattle, crows and camels, for example.
And then there's Staphylococcus aureus, a bacteria that's usually pretty harmless when found on our skin, as occurs among about 30 percent of our planet's human population. But when S. aureus penetrates that physical barrier to the microbial pathogens that coat us and float around us, it becomes a dangerous beast.
S. aureus can lead to life-threatening infections of our bones and joints, the linings of our hearts and the membranes surrounding our brains. In the blood, it can trigger the often lethal immune overreaction known as sepsis. In particular, S. aureus is one of the microorganisms that can organize into biofilms, slimy carpets of adherent cells that stick to prosthetic devices and are extremely difficult to eradicate. (The plaque clinging tenaciously to your teeth, however vigorous your efforts to brush it away, is a textbook example of a bacterial biofilm.)
Now toss in the increasing number of infections of growing numbers of prosthetic implants, increasing S. aureus-induced in-hospital infections, and increasing resistance of this microbe to common antibiotics, and the upshot is a major human health threat.
So it's good news that work by Stanford drug-development pioneer Matt Bogyo, PhD, and his colleagues has revealed a hitherto-unheralded class of potential drug targets in S. aureus that may provide a brand-new way of killing it off or, at least, dialing it down.
In a paper recently published in Nature Chemical Biology, Bogyo and company describe their use of a specialized screening process and subsequent unearthing and detailed characterization of a set of 10 previously overlooked enzymes that are found in S. aureus but not in humans (so a drug targeting such an enzyme might leave human cells unscathed). At least one of these enzymes, the team found, is crucial for establishing infection in key organs of mice (so, presumably, people as well). Block the enzyme, and the bacteria loses much of its ability to infect the heart, for example.
The fact that the enzymes seem to be pretty close to unique to Staphylococcus could make them ideal drug targets. One can imagine coating the surface of a prosthetic knee or hip-joint implants with such drugs to discourage the formation of S. aureus biofilms.
Plus, Bogyo tells me, "because they're so specific to staph bacteria, these enzymes could be used as biomarkers to image sites of staph infections in the body." His study showed that certain small fluorescent molecules have an affinity for the S. aureus-specific enzymes his team fingered. Fluorescence emanating from such a molecule bound to one of these enzymes could turn that enzyme into a beacon letting medical practitioners and researchers figure out just where in the body S. aureus cells are holed up and helping them gauge the success of, say, antibiotic treatments.
Photo by NIAID