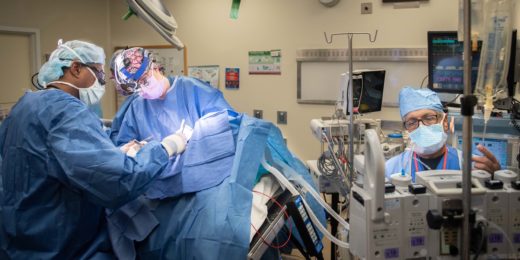
The United States is struggling with two interconnected epidemics — opioid abuse and chronic pain — says Sean Mackey, MD, Stanford's chief of pain medicine, and there are no easy solutions.
As Mackey and Ming-Chih Kao, MD, PhD, clinic chief at the Stanford Pain Management Center, note in an editorial in the British Medical Journal, 20 million Americans suffer from high-impact chronic pain, or pain so severe it impairs their daily lives. Medical advances, Mackey said, have allowed more people to live longer after surgeries, injuries and cancer treatments, all of which can produce persistent pain.
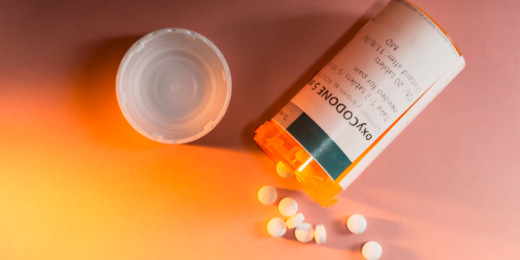
At the same time, they note, every day 130 Americans die from overdosing on opioids. Some of them became addicted after being prescribed opioids after surgeries or other procedures.
The number of people with chronic pain complicates the effort to curb the opioid epidemic — and vice versa. As Mackey and Kao write, restricting access to opioids may seem like a good idea, but preventing people with chronic pain from refilling their opioid prescriptions can not only cause them to live with severe pain but can lead them to suicide or abuse of illicit drugs such as heroin. Conversely, prescribing opioids too freely can set patients — or friends or family members who access leftover pills — on a path to addiction.
“There’s no one-size-fits-all solution,” Mackey said. “Pain treatment is highly individualized and personalized. I’ve prescribed opioids for chronic pain and seen that they can work long term. But I have taken other patients off them when it was clear they were causing harm.”
Mackey said that a host of tactics, outlined in the United States’ National Pain Strategy, are necessary to address both crises. They include pain psychology, use of non-opioid pain relief, physical therapy and alternative medicine techniques. The tactics emphasize prevention, notably keeping acute pain from developing into chronic pain.
The National Pain Strategy also stresses team-based interdisciplinary care, such as that used at the Pain Management Center, and better education about assessing, preventing and treating pain for all clinicians.
Mackey elaborated on a few of the strategies.
Because patients with severe psychological distress (for example, post-traumatic stress disorder, anxiety or depression) are more likely to develop addiction and chronic pain after surgery, he suggests that clinicians consider delaying elective surgery for patients until their psychological needs are addressed. “Let’s get them in the best psychological and physical state they can be in,” he said.
He also advocated reducing opioid prescriptions after surgery to better meet the needs of each patient. “Are we writing too many opioid prescriptions? The answer is obviously yes,” he said. Even when a patient takes only a few pills, he noted, the remaining opioids are sitting in a medicine cabinet, available to anyone in the house, such as teenagers who may take them to a party.
“Every patient’s needs are different, and some will require more opioids for a longer duration than others,” he said. “Our ultimate goal is to personalize this process by predicting the best treatment path for each patient and each surgery.”
And Mackey said it’s essential to intervene early, before pain becomes chronic: When pain lingers, it can become “a vicious cycle” in which the brain and the site of an injury maintain a communication loop, prolonging the pain. “You want to break that cycle as soon as possible,” he said, by treating the pain aggressively once it extends beyond the expected period of time.
None of these approaches alone will have much effect, he emphasizes. But taken together, he believes they will curb opioid abuse while allowing patients to use opioids when they need them.
“If we address the goals in the National Pain Strategy,” he said, “it’s going to have a big impact on the dual crises of pain and prescription opioid abuse.”
Photo by Raj Eiamworakul