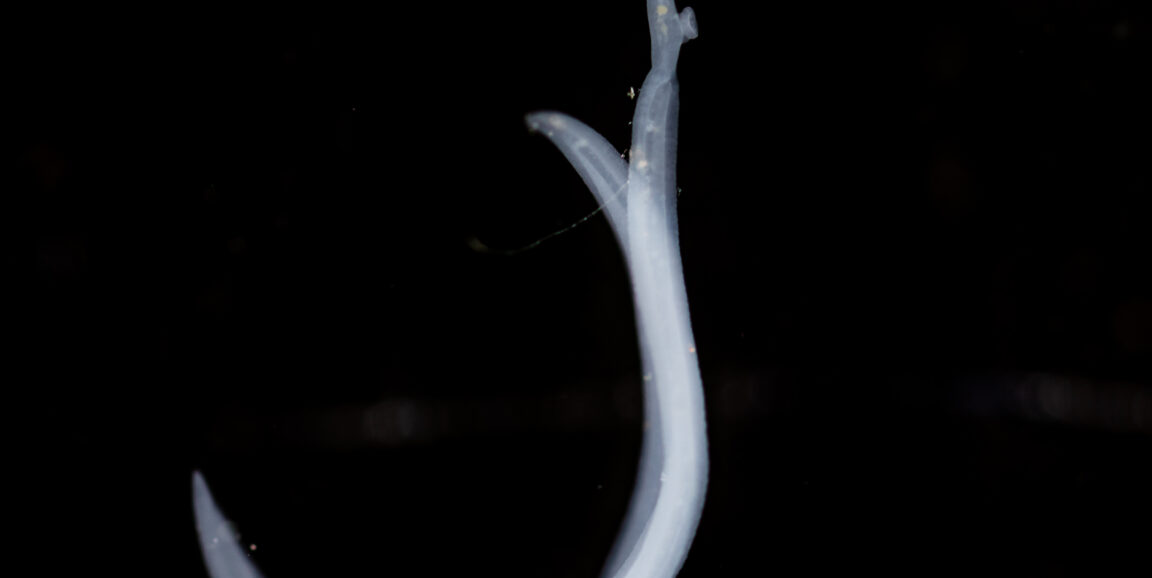
Think you've seen unattractive couples before? If you look up, you'll have the pleasure of viewing the ugliest couple you've ever seen: a male and female of the trematode-worm species Schistosoma haematobium, caught in flagrante delicto. The result of this union is likely to be several hundred eggs per day, deposited in the bladder wall of any one of the conservatively estimated 112 million people with urogenital schistomiasis.
That's a lot of people. Plus, each worm can live for years or decades comfortably ensconced in the blood vessels marbling the bladder wall. So we're talking chronic. The sole drug (praziquantel) approved for this condition works imperfectly and tastes terrible. That's a gourmet's-dream recipe for eventual drug resistance, which means this compound's days are numbered.
In fact, if you consider the overall health effect as measured by so-called quality-adjusted life years, which assesses disease burden in terms of both loss of life and damaged health among the living, schistosomiasis ranks right up there with malaria as a world-class tropical scourge, according to Stanford urologist Mike Hsieh, MD, PhD. Like malaria, schistosomiasis is as under-understood as it is widespread.
Among the many reasons for this, one is that until quite recently there has been no decent animal model for S. haematobium infection, which in humans targets the bladder. If you infect rodents with these parasites, they head for the liver and intestine instead. But Hsieh has come up with an improved model in which S. Haematobium eggs are injected directly into the bladder wall, not only mimicking the human outcome but providing a metronome, as it were: One knows exactly when the infection clock started ticking.
By synchronizing the initiation of infection in experimental mice, an experimenter can perform multiple analyses to find out which specific genes in infected bladder tissue are amped up or tamped down over time, resulting in a series of "snapshots" of the infection's effects on the tissue. That's what Hsieh did, in a study just published by the journal PLoS - Neglected Tropical Diseases.
Hsieh's team saw activation of clusters of genes inplicated in fibrosis (scarring, which can cause kidney failure) and carcinogenesis (for which schistosomal bladder infection is a risk factor), and a downshift among genes charged with maintaining bladder-wall integrity (which could explain the leakage of schistosome eggs into the urine and the subsequent cycle of constant contamination).
In my release about this study, I quoted Hsieh as saying it would have been impossible to see this simply by observing patients, because there would be no way to pool their samples to study the time-course of changes in gene-activation levels:
"With the natural human infection, you never know when any given person is initially infected--unless it's that unfortunate American tourist that got infected while swimming in Lake Victoria on a weeklong Africa visit," he said.
Previously: A good mouse model for a bad worm, Neglected story of schistosomiasis in Ghana, as told in a sand animation and Compound clogs Plasmodium's in-house garbage disposal, hitting malaria parasite where it hurts
Photo by sinhyu