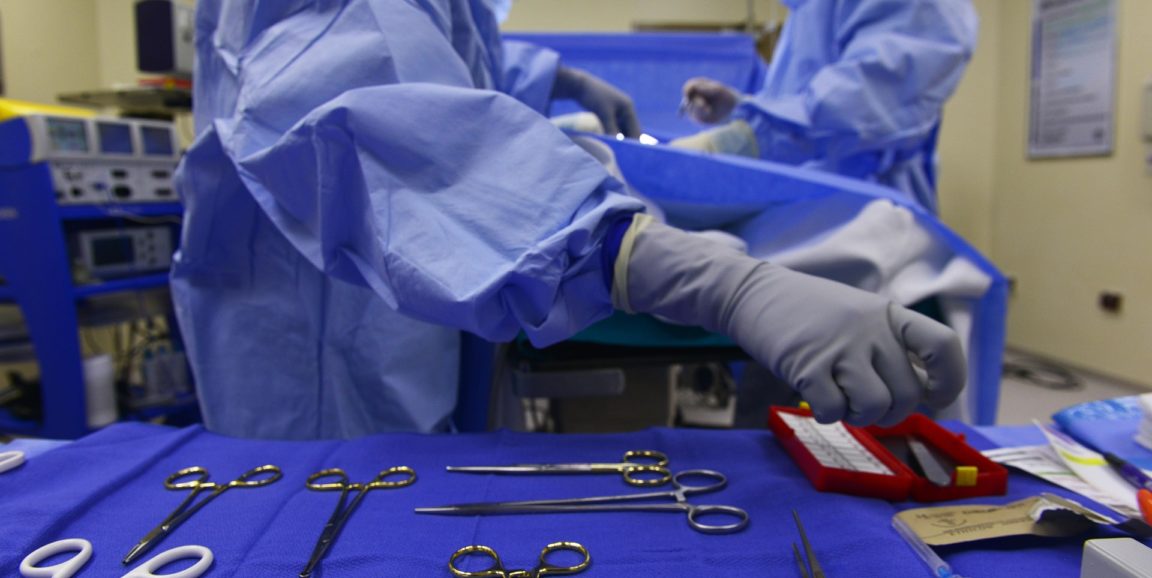
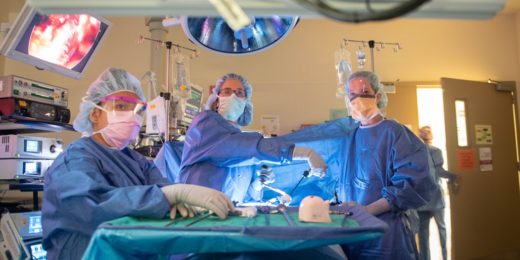
When Kathleen Wilde was first diagnosed with breast cancer in 1999, her doctors were able to successfully treat the disease without removing her breasts.
However, a biopsy in July revealed that cancer had returned in an invasive form. Wilde, a nurse and patient advocate from Pismo Beach, California, knew she needed a mastectomy; but she also realized that she didn't have sufficient body fat in her lower abdomen for the traditional reconstruction.
Her surgical oncologist, Irene Wapnir, MD decided to explore an entirely new approach: implants using omentum, a curtain of fatty tissue that hangs from the stomach and wraps around the internal organs.
"Omentum is used by plastic surgeons to cover wounds or other defects in the body routinely," said Wapnir, who is a professor of surgery at Stanford. "Our challenge was to implement it for a different indication."
Typically, after removing all of a patient's breast tissue in a mastectomy, plastic surgeons reconstruct the breast using blood vessels known as deep inferior epigastric perforators, or DIEP, from the lower abdomen, along with skin and fat from that region. The procedure is referred to as the DIEP flap.

Traditionally, patients who aren't candidates for DIEP flap have only one other option: artificial implants. However, Wapnir, was hesitant to suggest this avenue for Wilde because of recently-raised concerns about a possible connection between silicone protheses and anaplastic large cell lymphoma.
To help develop the new technique, Wapnir recruited Dung Nguyen, MD, PharmD, a breast reconstructive surgeon. "One of the challenges with using omentum is that it is a formless sheet; in other words, it does not have a solid shape," Nguyen said.
In the implant that Nguyen designed, the omental flap would provide blood flow to the tissue, while grafted fat would provide volume. Soft, connective tissue called acellular dermal matrix would serve as a casing, allowing Nguyen to shape the tissue into a mound and create a breast with a natural look and feel.
For Wilde's procedure, three surgeons worked simultaneously, allowing her to be under anesthesia for a shorter period of time.
Yulia Zak, MD, a minimally-invasive surgeon, harvested the omentum laparoscopically, allowing Wilde to avoid taking narcotic pain-reducers after the operation. While Zak removed the omentum, Wapnir performed a nipple-sparing mastectomy and Nguyen harvested fat from the patient's thighs. After the breast tissue had been removed, Nguyen set to work creating the biological implant. Through microsurgery, she then vascularized the entire biological implant by connecting blood vessels from the omentum to the patient's chest.
Wapnir said she was encouraged by how the procedure went for Wilde and excited by the potential benefit for other patients. With Nguyen and the rest of her team, she plans to do additional "biological implant" breast reconstructions and document long-term cosmetic outcomes.
"We pride ourselves on aiming to achieve a normal appearance for every woman who needs or chooses to have a mastectomy," she said. "I believe this is an innovative breakthrough that may be associated with quicker recovery, less pain and better outcomes all around."
For her part, Wilde said she was happy with her results: "I'm glad I could help future patients in a similar situation," she said.
Top photo by skeeze; Middle photo courtesy of Irene Wapnir.