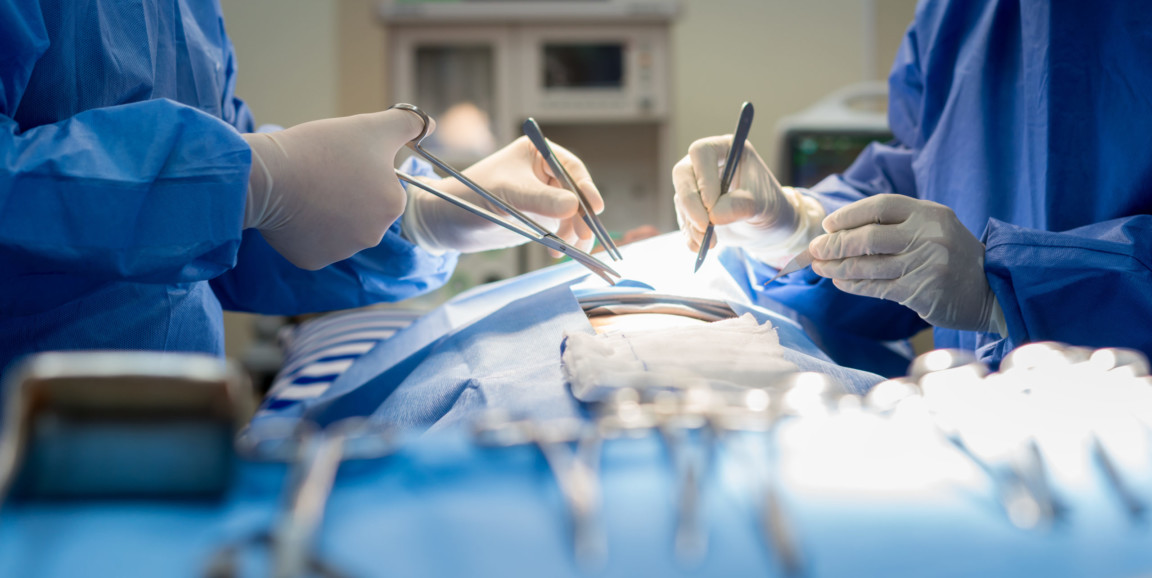
A boxing fight and a surgical operation don't take exactly the same physical toll on a person's body. But Brice Gaudillière, MD, PhD, a Stanford Medicine associate professor of anesthesiology, pain and perioperative medicine, sees some similarities in how a fighter and a patient might think about the big event.
"Let's put it this way: Would you want to go in the ring with Mike Tyson tomorrow, or would you get in shape first?" he asked.
Of course, the answer is get in shape. The same applies for going under the knife -- especially for patients who have a higher risk of post-surgical complications.
Patients who can prepare their body before surgery -- whether that means eating better, undergoing physical therapy or something else -- often have smoother recoveries and fewer complications. But there's a catch.
"If you are about to have a surgery today, a surgeon really cannot give you an accurate estimate of the chances you'll have a complication," said Gaudillière. "They occur at a fairly high rate, and they can be devastating."
Now, Gaudillière and co-senior authors Cindy Kin, MD, assistant professor of surgery; Martin Angst, MD, professor of anesthesiology, perioperative and pain medicine; and Nima Aghaeepour, PhD, assistant professor of anesthesiology, perioperative and pain medicine, have led a national study showing that a blood-based test they developed can predict which patients are at higher risk of surgical complications, such as infection, and therefore will benefit the most from getting in shape for an upcoming surgery.
Research fellow Kristy Rumer, MD, PhD; data analyst Julien Hedou; researcher Amy Tsai, MD; and postdoctoral fellow Jakob Einhaus, MD, PhD, share lead authorship of the study, which was published in the Annals of Surgery.
Pre-surgery preparation
For non-emergency surgeries, patients typically meet with a surgeon and an anesthesiologist two to six weeks before the procedure, allowing plenty of time to perform a predictive test, such as the one Gaudillière and his team developed, and provide tailored advice on how best to avoid complications, Gaudillière said.
The test, which probes a patient's immune response, could help surgeons better plan the timing of surgeries and choose the best surgical approach. It could also help clinicians tailor immune-boosting interventions for patients before surgery to improve healing and recovery. That could be a "prehabilitation" regimen that includes better nutritional habits, physical therapy and meditation, said Gaudillière. The test could become available to surgical patients at Stanford in two to five years.
Predicting risk
During the study, 41 patients underwent abdominal surgery to remove non-cancerous bowel tissue, a procedure typically performed to treat bowel blockage, bleeding or severe inflammatory bowel disease. Surgical site complications, such as infection or a tear or rupture of the surgical site, are relatively common with the procedure, Gaudillière said, affecting 15% to 25% of patients.
Researchers wanted to study how each patient's immune system responded to surgery, as the immune system guides many aspects of a patient's recovery, including protection against infections, pain improvement and wound healing. The team drew blood from patients before and 24 hours after surgery, then ran lab tests measuring the activity of millions of immune cells.
Gaudillière and other researchers inspected both the pre- and the post-surgical samples. They first looked at the immune responses triggered by the trauma of surgery. There are two phases in the immune response to surgery: The first promotes inflammation and is triggered immediately when the injured tissue releases "danger-signals" that tells the immune system the skin has been broken and infectious pathogens can enter the body. The second phase tamps down the immediate inflammation, responds more specifically to bacterial threats, and plays an important role in wound healing and the decrease of pain post-surgery.
The team found that patients who suffered surgical site complications after surgery were often those whose immune responses had levels of inflammation that were either too high or too low.
The researchers also wanted to find out whether immune responses measured before surgery could predict which patients developed surgical site complications after surgery. They developed a blood test designed to mimic the trauma experienced by the body during surgery, prompting an immune response similar to what might occur during and after an abdominal surgery. Results from this pre-operative "immune stress test" showed that the blood test's results were largely aligned with how the patients' immune system responded after surgery and accurately identified patients who developed complications.
Gaudillière said he hopes their discovery will allow doctors to draw a patient's blood before surgery, run it through this battery of tests, and use the results to predict who might suffer complications and how to offset them.
Expanding testing
In the study, patients' immune system responses predicted surgical site infections with about 84% accuracy. While that means that about 16% of patients' complications might not be predicted correctly, over 80% accuracy is much higher than that of other predictive tests currently available, Gaudillière said.
He said more work must be done before the predictive blood tests can be used in a patient population with the diverse ages, races, physical fitness levels, pre-existing conditions and other differentiating factors. Additional studies also are needed to verify whether these findings will translate to other surgical procedures.
But if they do, patients receiving surgery at Stanford could benefit from more personalized surgery plans, with lifestyle changes or therapies put in place before surgery to help prevent post-surgical infection.
"You can prepare a patient differently for surgery if you know a patient's risk for developing complications," Gaudillière said. "If you can predict, you can prevent."
Photo by ake1150