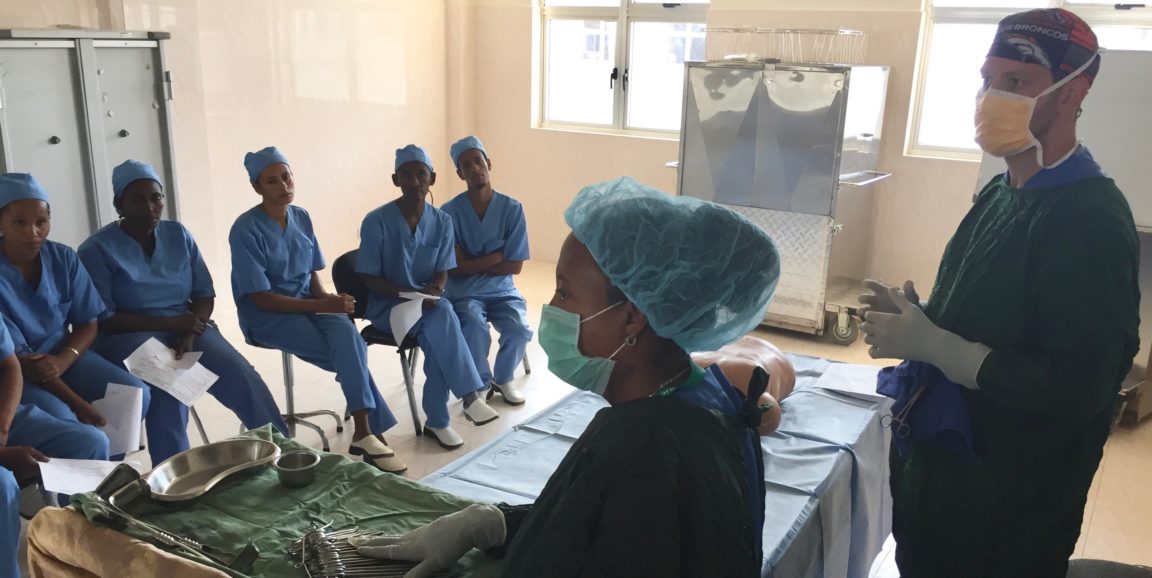
After an inspirational experience working with a family medicine doctor in Nepal as a medical student, Jared Forrester, MD, knew he wanted to spend more time focusing on global health during his surgical residency at Stanford Medicine.
He discussed it with Thomas Weiser, MD, MPH, who was the mentor for his internship class. Known for his role helping to create the World Health Organization's Surgical Safety Checklist, Weiser was now a consulting medical director at the nonprofit Lifebox. He suggested a professional development project working on the ground in Ethiopia to create a surgical infection prevention plan.
Forrester was game. He signed on, and in July 2016, he began his two-year stint in Ethiopia.
Leading cause of complications in surgical patients
Surgical site infections are a leading cause of complications and death in patients who have had operations, particularly in low and middle-income countries. In 2018, GlobalSurg Collaborative reported that infection rates following gastrointestinal surgery were 23% in low-income countries--nearly twice that of high-income countries.
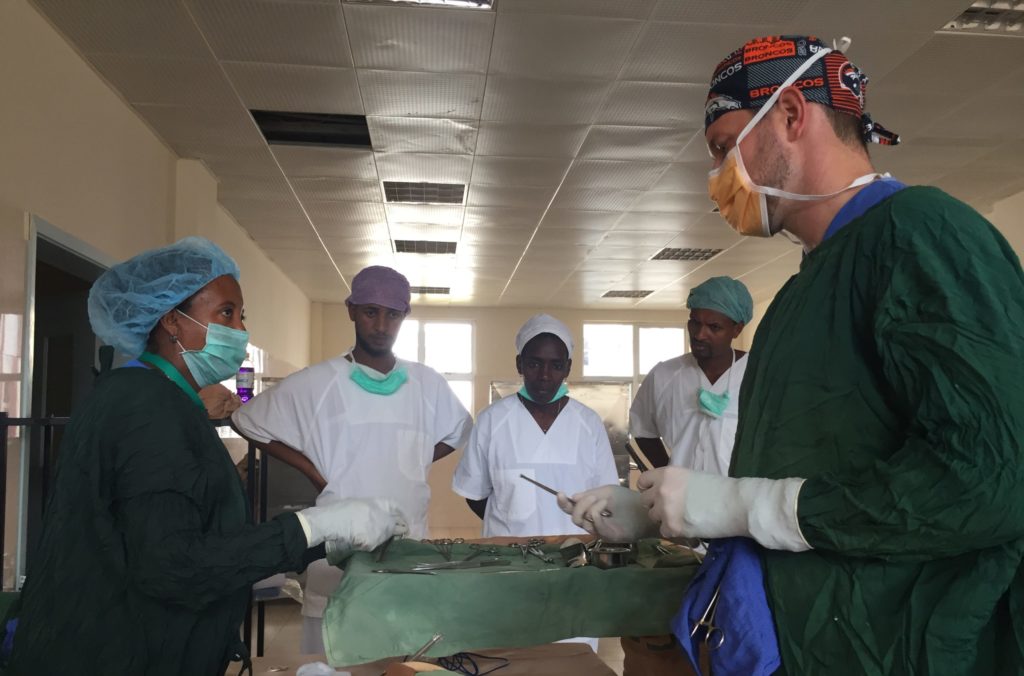
Forrester says that's the result of three different factors: the pathogen, the patient, and surgical processes. "Pathogen factors" include how resistant certain bacteria are to antibiotics or the degree of contamination the wound. "Patient factors" include delay in access to surgical care but also patients who are immunicompromised due to conditions, such as obesity or HIV. "Surgical factors" -- lapses of sterilization during an operation -- is the area in which Forrester decided he could make the most impact.
Forrester spent his first few weeks in Jimma observing and meeting surgeons, anethesthiologists, nurses, and hospital administrators.
"I needed to learn, build trust and then get buy-in for any changes we wanted to try putting into action," said Forrester.
A surgical safety checklist for low-resource settings
Forrester knew he couldn't just implement the surgical safety checklist; a 2013 study published in BMJ showed that compliance with the list in low and middle-income countries is handicapped by resource limitations, including nurse and supply shortages. He decided to break down the problem to understand it better, even following a sterile instrument through its entire life cycle to determine at what points it could become contaminated.
After a couple months, Forrester had narrowed the scope of his project down to six focus areas: hand and surgical-site skin antisepsis; ensuring integrity and sterility of gowns, drapes and gloves; instrument decontamination and sterilization; timing and selection of prophylactic antibiotics; routine surgical gauze counting; and routine use of the Surgical Site Checklist, focusing on the communication aspects. His scope was narrower than the 19-item checklist's resource-heavy requirements because he wanted to providers to focus on safety, improving teamwork, and building infrastructure.

Forrester implemented the six surgical site infection prevention standards by first establishing a system to ensure compliance and compiling baseline data on infection rates. He also led process-mapping exercises to determine gaps in their current processes. Teams then met every few months to review progress and identify areas for further improvement. For example, one hospital established a procedure to mend holes in gowns and another mandated including sterility indicator tape in instrument trays.
Forrester relocated in his second year to the capital, Addis Ababa and worked to refine the project down to "something that could be taught, rolled out, and driven by the excellent clinicians and nursing staff with ongoing support by a surgical fellow." Lifebox dubbed it the Clean Cut Program.
Promising early results
Early results of Forrester's work were recently published in the British Journal of Surgery.
He and his colleagues collected data on more than 2,000 operations. They found that the number of surgical site infections dropped an average of 35% across five facilities using the program. Facilities with the highest compliance with the Clean Cut Program showed the most improvement.
"I think if we showed a 35% drop in infection rate from an antibiotic, we'd call it a miracle drug," Forrester said. "It just goes to show that when we work as a team, we can affect big change. It doesn't require huge monetary investment, but it does require human buy-in to strengthen systems and make a difference."
After Forrester returned to the United States in October 2016, Nichole Starr, MD, MPH, a resident at the University of California, San Francisco, took over the next phase of the Clean Cut Program. Starr rolled out the program to numerous other hospitals in Ethiopia, but her work was put on hold earlier this year due to the pandemic.
Back at Stanford, Forrester has worked with his program directors and mentors to shape the rest of his residency to prepare for a career as a surgeon in more austere settings. That included a rotation in Zimbabwe with Sherry Wren, MD, winner of the 2017 American College of Surgeons' Surgical Humanitarian Award; and another with the obstetrics/gynecology department to learn how to perform a Cesarean section, one of the most common operations abroad.
Forrester's fiancée completes her fellowship in abdominal transplantation this year, so he says his next steps will follow hers. Wherever he lands, he hopes to continue serving underresourced and overlooked populations.
"I've been very blessed and fortunate in life," Forrester said, "and I think it's important to give back."
Photos courtesy of Jared Forrester.