The COVID-19 pandemic provided the first taste of telemedicine for many people, but Jodi Prochaska, PhD, has been harnessing the benefits of virtual health care for several years.
Prochaska, a researcher at the Stanford Prevention Research Center who specializes in tobacco reduction, is one of the leaders of the Healing and Empowering Alaskan Lives Toward Healthy Hearts, known as HEALTHH, project in Alaska. The project examines how telemedicine can improve heart health for Alaska Native men and women who use tobacco.
Prochaska has been working in Alaska since 2009, when she was invited to teach best practices to local clinicians and public health workers in Anchorage by the Alaska Native Tribal Health Consortium. That work led to a collaboration beginning in 2015 in the Norton Sound region of Alaska.
There's a high prevalence of smoking in Alaska particularly among the Native population. About half of Alaska Native men and a third of Alaska Native women smoke -- rates that haven't been seen in the continental United States since the 1960s.

"It's a very high smoking prevalence in a remote location, without easy access to treatment. Developing partnerships and trust is critical," Prochaska said. To that end, the study team partnered with the tribal council in the Norton Sound region.
Prochaska's "incredibly multidisciplinary" team includes cardiologists, pharmacologists, experts in nutrition and exercise science, and students, trainees and research staff members as well as Prochaska, who is a clinical psychologist.
Exercise and Native diet
This team created the HEALTHH study: a two-group randomized controlled trial.
Working in small communities, all study participants receive active counseling interventions. One group is focused on tobacco and physical activity; the other is focused on Native diet and heart medication compliance. The project aims to examine changes in individual behaviors such as smoking and in overall quality of life over 18 months.
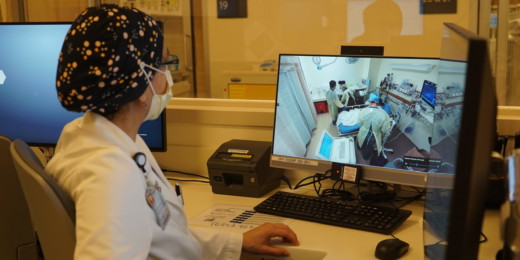
These interventions are largely delivered by telemedicine. "Telemedicine enabled direct contact to the communities," Prochaska said.
All the study participants received telemedicine counseling from counselors based in Anchorage and Stanford. They were also mailed a study manual with either a pedometer and nicotine replacement therapy or a heart-healthy Native cookbook and medication bag. Telemedicine sessions were provided at baseline and at three, six, and 12-months.
The results of the project haven't been published yet, but receptivity was high among participants, Prochaska said.
"I found it very helpful," one anonymous participant said. "A lot of people don't have enough information about [the dangers of smoking], and like learning how long it takes for the body to heal itself and different practices to ease those cravings."
Participants were asked if they'd recommend the program to a friend, and how highly they'd rate it on a scale of 1 (low) to 10 (high); participants were generally enthusiastic, she said.
Telemedicine counseling was given an average rating of 8.7 across all age ranges of participants, with both men and women rating it above an 8. The accessibility of telemedicine (particularly now) makes this an exciting prospect for the future, Prochaska said.
"You guys really helped me with trying to quit smoking," another participant said. "There was a lot of different opportunities to quit and that helped me out a lot."
Photos courtesy of the HEALTHH team