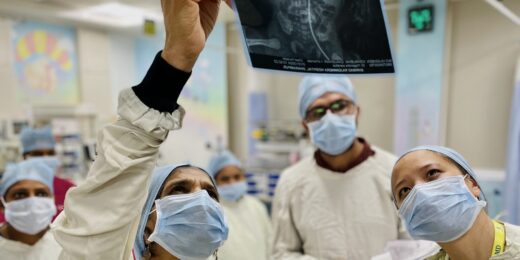
The goal of a decade-old program started by Stanford Medicine's Nilima Ragavan is to foster the sharing of lessons and evidence-based best practices between clinicians in the U.S. and India.
Category: Pediatrics
Inequity of genetic screening: DNA tests fail non-white families more often
Research is showing that advanced methods of genetic testing aren’t equally useful for everyone: They’re less accurate for non-white families, raising concerns about how historical gaps in whose DNA gets studied produce inequities in medical care.
Imagining virtual reality as a simple tool to treat depression
Some of the 17 million Americans afflicted with major depressive disorder each year may soon receive a surprising new prescription from their clinician: Have fun on a virtual reality device.
Why precision medicine’s targeted interventions may help prevent dangerously early births
Approximately 10% of babies worldwide are born three or more weeks before their due date -- making premature birth the leading cause of death for children under 5 globally.
Sick of being sick? As respiratory viruses roar back, experts offer guidance
Nationwide, the percentage of health care visits for flulike symptoms ticked up above the baseline at the start of November and has remained elevated ever since, according to the Centers for Disease Control and Prevention.
More kids are being hospitalized for eating disorders — researchers learned why
Over the last decade, physicians have taken a broader view of adolescent eating disorders, thanks to a growing recognition of the variety of disordered eating patterns that can harm patients’ health, especially their heart function.
Researchers seek healthy checks and balances for how products are designed
With such conveniences as digital devices at our fingertips comes a messy health conundrum, say Stanford Medicine researchers.
The endometriosis enigma: What to know about this disruptive disease
Despite the fact the disease greatly reduces the quality of many women’s lives, endometriosis remains understudied.
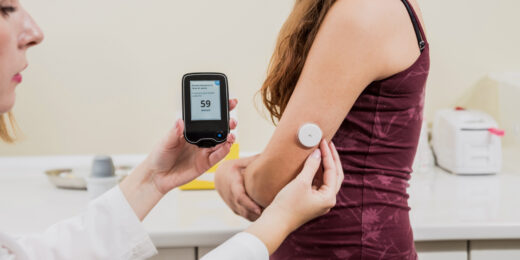
Why precision medicine leads to better diabetes care
Improvements in treatment technology are helping physicians deliver individualized care to their Type 1 diabetes patients.
What one youth mental health expert wants you to know about suicide
September is Suicide Prevention Month and mental health experts at Stanford Medicine have important information to share.
No more ‘just deal with it’: Helping teens have easier periods
Nichole Tyson, MD, has advice for young people seeking help for menstrual problems – including painful, irregular or heavy periods.
How to safeguard teens’ well-being on social media
A Stanford Medicine expert has tips for parents wondering how to help teens balance mental health concerns and social media use.
Brain cancer specialists hope Biden’s Moonshot speeds therapies
Stanford Medicine brain cancer researchers joined other thought leaders in Washington, D.C. to discuss what the Biden Administration-led Cancer Moonshot initiative could mean.
Photos shine light on pediatric medical experience
Pediatric patients and their parents capture their experiences at Lucile Packard Children's Hospital Stanford, sharing photos in an exhibit.
This Is My Why: Champions of Stanford Medicine hospitals
We're celebrating those who contribute to the success of Stanford Medicine's hospitals through unwavering passion and dedication.
Kids’ storybooks encourage more water, less sugary drinks
Researchers at Stanford Medicine are finding creative ways to entice kids into drinking more water and less sugary drinks.